What is denial management?
Denial management includes tracking denial trends, finding root causes, and improving workflows to prevent the same issues from happening again. This process helps healthcare providers keep more of their money, improve cash flow and make billing more efficient overall.
In short, denial management isn't just about fixing denied claims — it's also about making the system better so that fewer claims are denied in the future.
Medicare and private insurance companies look over claims for medical services, supplies or procedures before paying them. Denial management helps fix the problem by correcting, resubmitting or appealing a claim that was denied.
What is denial management in healthcare?
In healthcare, denial management means all the work that providers do to lower the number of claim denials and raise the amount of money they collect. It links together different parts of the revenue cycle — registering patients, checking insurance, coding, documentation, submitting claims and following up with payers.
Errors often lead to denials even before the claim is filed. Denial management requires the involvement of individuals from diverse departments.
It is a structured process that helps healthcare organizations figure out why a claim was denied, fix the problem and get the money back by resubmitting or appealing. Finding problems that happen repeatedly — like eligibility mistakes, missing authorizations, coding errors, incomplete paperwork and late filing — is also a key part of denial management.
Denial management is important in healthcare because it protects income, improves cash flow, cuts down on administrative work and supports the overall revenue cycle. It's not enough to fix denied claims after they happen — you also need a system that stops them from happening in the first place.
What is denial management in medical billing?
Denial management in medical billing is the process of handling claims that have been denied or left unpaid by insurance companies. It helps billing teams figure out why the payment was denied, fix the problem and take the necessary steps to recover the money.
![]() 7 key points of managing denial in medical billing:
7 key points of managing denial in medical billing:
 Review claims that were denied
Review claims that were denied Find out why the denial happened
Find out why the denial happened Fix mistakes on claims
Fix mistakes on claims Resubmission or appeal of a claim
Resubmission or appeal of a claim Follow-up with the payer
Follow-up with the payer Analyze the trend of denials
Analyze the trend of denials Protect revenue
Protect revenue
What is denial management in revenue cycle management (RCM)?
Denial management is an important part of revenue cycle management that keeps provider revenue safe. It works after a claim has been denied, but how well it works depends on earlier steps in the RCM process — checking eligibility, getting authorization, coding and keeping records.
Good denial management helps the whole revenue cycle by cutting down on rework, speeding up payments and making it easier for claims to be accepted the first time.
What is the fundamental approach to managing claim denials?
The basic approach to denial management includes five important steps. Each step helps healthcare providers fix denied claims, recover payments and reduce future denials.
![]() Finding out why it was denied
Finding out why it was denied
Carefully read the denial code and the payer's response. This helps the team figure out exactly why the claim was turned down.
![]() Sort the denial by type and reason
Sort the denial by type and reason
Once the reason is known, it is placed into one of the following groups — eligibility, authorization, coding or documentation. This makes it easier to spot patterns and identify the real root cause of repeated denials.
![]() Fix the problem
Fix the problem
The billing team fixes the mistake by updating claim details, adding missing documents or correcting codes. This step makes the claim ready for successful reprocessing.
![]() Resubmit or contest the claim
Resubmit or contest the claim
The corrected claim is sent back to the payer if the denial was based on a fixable mistake. An appeal is filed with supporting information if additional proof is required.
![]() Stop the same problem from happening again
Stop the same problem from happening again
Analyze denial trends and improve internal processes to cut down on recurring mistakes and make the billing process more proactive.
This method helps providers stop just reacting to denials and start making the revenue cycle process more accurate and efficient.
What is the denial management process?
A standard denial management process is a step-by-step way to fix, track and stop insurance claims from being denied. It helps healthcare providers get paid, cuts down on problems with repeated claims and makes the whole revenue cycle work better.
![]() Finding out about the denial
Finding out about the denial
The process starts when the payer denies a claim and the filer gets the denial through remittance advice, payer portals, explanation of benefits or electronic claim responses. The billing team reviews the denial message carefully to confirm the claim needs action.
![]() Putting denials into groups
Putting denials into groups
Once the denial is found, it is categorized based on the reason — eligibility, authorization, coding, medical necessity, documentation or timely filing. Proper categorization helps track which problems occur most often.
![]() Finding the root cause
Finding the root cause
The next step is to figure out exactly where and why the problem happened. This could mean looking for mistakes in patient registration, insurance verification, coding accuracy, physician documentation, charge entry or claim submission.
![]() Fix the claim
Fix the claim
The billing team fixes the mistakes by updating patient information, correcting codes, adding modifiers, attaching missing documents or making any other necessary changes. A small mistake left uncorrected could trigger another denial.
![]() Resubmission or appeal
Resubmission or appeal
If the denial is due to a small mistake, the corrected claim is resubmitted to the payer. If more explanation or proof is needed, the team submits a formal appeal with the right documentation by the payer's deadline.
![]() Follow-up
Follow-up
After resubmitting or appealing, the team checks in with the insurance company regularly to monitor the claim's progress. This step ensures claims don't stay open too long and helps receive payment faster.
![]() Prevention
Prevention
The last step is to analyze denial trends and recurring problems to ensure they don't happen again. Providers use this information to improve workflows, train staff and make the billing process more accurate.
The denial management process is not just about fixing denied claims after they happen. It also aims to strengthen the system to prevent future claim denials and safeguard healthcare revenue.
What are the common types of claim denials?
Some of the most common denial types include:
 Eligibility denials
Eligibility denials Prior authorization denials
Prior authorization denials Coding denials
Coding denials Medical necessity denials
Medical necessity denials Duplicate claim denials
Duplicate claim denials Timely filing denials
Timely filing denials Missing documentation denials
Missing documentation denials Coordination of benefits denials
Coordination of benefits denials Non-covered service denials
Non-covered service denials Demographic error denials
Demographic error denials
What are the root causes of claim denials?
![]() Incorrect patient information
Incorrect patient information
Wrong details — like the patient's name, member ID or policy number — can cause immediate denial. Even a small registration mistake can delay or deny payment.
![]() Insurance eligibility not verified
Insurance eligibility not verified
If the patient's coverage is not checked before the service, the claim may be denied because the policy is inactive, expired or does not cover the treatment. Checking eligibility is one of the most important steps in preventing denials.
![]() Missing or invalid authorization
Missing or invalid authorization
Many treatments and procedures require advance insurance approval. If authorization is not received, has expired or was entered incorrectly, the payer may deny the claim.
![]() Coding mistakes
Coding mistakes
Wrong diagnosis codes, procedure codes or billing codes can result in a denied claim. Payers use these codes to determine if a service is billable and covered, so accuracy is critical.
![]() Incomplete clinical documentation
Incomplete clinical documentation
If medical records don't clearly show that treatment or service was given, the payer may deny the claim. Proper documentation is essential to prove medical necessity and receive reimbursement.
![]() Late claim filing
Late claim filing
Each payer has a filing deadline. Claims submitted after the deadline are automatically denied regardless of whether the service was valid.
![]() Duplicate submissions
Duplicate submissions
Submitting the same claim more than once — whether intentional or accidental — results in a duplicate denial, delaying or preventing payment.
What are effective denial management strategies?
![]() Checking insurance before the visit
Checking insurance before the visit
Verifying a patient's insurance eligibility before their visit confirms the policy is still active and what services are covered. This cuts down on denials caused by inactive coverage, benefit issues or incorrect insurance information.
![]() Getting the right authorizations
Getting the right authorizations
Before some treatments can be performed, the payer must give approval. Missing, expired or incorrectly entered authorizations can result in denied claims.
![]() Improving the quality of documentation
Improving the quality of documentation
Clear and complete clinical documentation shows that the service was needed and performed correctly. Proper documentation helps ensure coding accuracy and reduces denials based on missing information or lack of medical necessity.
![]() Editing claims before submission
Editing claims before submission
Claim edits help identify common mistakes before the claim reaches the insurance company — reviewing codes, modifiers, patient information and billing rules so that issues are resolved immediately.
![]() Monitoring denial trends regularly
Monitoring denial trends regularly
Analyzing denial patterns helps providers understand the most common problems and why they happen. This makes it easier to fix recurring issues, improve workflows and reduce future denials.
What are the best practices for claims denial management in healthcare?
 Verify patient eligibility every visit
Verify patient eligibility every visit Collect complete and accurate patient data
Collect complete and accurate patient data Secure prior authorization before services
Secure prior authorization before services Ensure coding accuracy
Ensure coding accuracy Improve physician documentation
Improve physician documentation Track filing deadlines carefully
Track filing deadlines carefully Assign denial ownership clearly
Assign denial ownership clearly Review top denial reasons monthly
Review top denial reasons monthly Perform regular staff training
Perform regular staff training Create preventive action plans based on denial trends
Create preventive action plans based on denial trends
A strong denial management program combines prevention, correction, reporting and accountability.
What are the key denial management KPIs?
Denial management KPIs are key performance indicators that show how well a healthcare organization is dealing with denied claims. These numbers help monitor denial trends, find problem areas, improve collections and stop revenue loss.
![]() Rate of initial denial
Rate of initial denial
This shows how many claims are turned down the first time they are sent in. A high initial denial rate usually means that there are problems with checking eligibility, coding, getting permission or submitting claims.
![]() Rate of final denial
Rate of final denial
This tells you what percentage of claims are still unpaid even after you try to resubmit or appeal them. It helps providers figure out how much money they will never get back because of denials that aren't resolved.
![]() Denial based on reason
Denial based on reason
This metric keeps track of the most common reasons for denials, like coding mistakes, missing authorization or incomplete paperwork. It helps teams find problems that keep happening and fix them.
![]() Payer denials
Payer denials
This tells you which insurance companies turn down the most claims. It helps providers learn about the rules for each payer and how to bill better based on those rules.
![]() Rate of appeal
Rate of appeal
This is the percentage of denied claims that are formally challenged. It shows how often the organization is trying to get money back from claims that were denied.
![]() Rate of success for appeals
Rate of success for appeals
This shows how many claims that were appealed are successfully overturned and paid. A higher success rate for appeals means that the documentation is good, the follow-up is correct and the denial management is effective.
![]() Days until the problem is fixed
Days until the problem is fixed
This KPI shows how long it usually takes to settle a claim that has been denied. Faster resolution means the organization gets its money back faster and improves cash flow.
![]() Rate of preventable denial
Rate of preventable denial
This shows how many denials were caused by mistakes in the company's internal processes, like mistakes in registration, coding or missing documents. It helps providers focus on prevention and improving their workflow.
![]() Rate of clean claims
Rate of clean claims
This shows the percentage of claims that are accepted and processed without being turned down the first time they are submitted. A high clean claim rate means the billing process is accurate and efficient.
What is the industry benchmark for denial management?
Benchmarks can change based on specialty and payer mix, but in general:
 A lower denial rate is always better
A lower denial rate is always better Strong organizations aim for a high clean claim rate
Strong organizations aim for a high clean claim rate An efficient team resolves denials quickly
An efficient team resolves denials quickly A lower write-off rate indicates stronger recovery efforts
A lower write-off rate indicates stronger recovery efforts High appeal success means follow-up and documentation support are satisfactory
High appeal success means follow-up and documentation support are satisfactory
Providers should not just compare their performance to the industry average — they should track their own progress every month and work to improve continuously.
What does a denial management workflow look like?
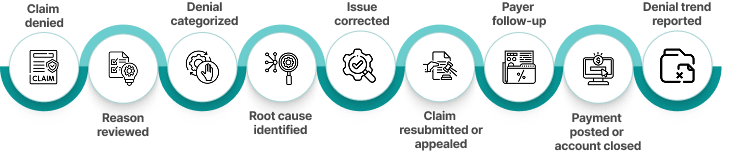
What are denial management reports?
Denial management reports are used to track how well denial management is working and to find recurring patterns in healthcare billing. They typically include:
 Total number of denied claims
Total number of denied claims Most common reasons for denial
Most common reasons for denial Number of denials by payer, provider or department
Number of denials by payer, provider or department Number of appeals filed and success rate
Number of appeals filed and success rate Age of denials and outstanding balances
Age of denials and outstanding balances Write-offs and unrecovered amounts
Write-offs and unrecovered amounts Patterns of repeated denials over time
Patterns of repeated denials over time
These reports help healthcare organizations identify where problems are occurring, improve follow-up efforts and make better decisions to improve revenue cycle performance.
What is the claims appeal process in denial management?
A provider can use the appeal process if they believe a denial is wrong or can be challenged. It usually involves:
![]() Reviewing the denial reason
Reviewing the denial reason
Carefully read the denial code and payer's explanation to understand exactly why the claim was rejected.
![]() Checking payer rules and filing limits
Checking payer rules and filing limits
Each payer has specific appeal deadlines and documentation requirements that must be met.
![]() Gathering the right paperwork
Gathering the right paperwork
Collect medical records, authorization details, coding support and any other documentation that supports the appeal.
![]() Writing a letter of appeal
Writing a letter of appeal
Draft a clear, professional appeal letter explaining why the denial should be overturned with supporting evidence.
![]() Submitting the appeal on time
Submitting the appeal on time
File the appeal before the payer's deadline to preserve the right to payment.
![]() Following up until a final answer is received
Following up until a final answer is received
Regularly check in with the payer to track appeal status and ensure no claim is left unresolved.
A good appeal process can recover significant revenue that would otherwise be lost.
How can healthcare organizations reduce claim denials?
![]() Verifying insurance in advance
Verifying insurance in advance
Checking a patient's insurance before they arrive confirms the policy is active and what services are covered. This prevents denials caused by inactive coverage, coverage limits or incorrect information.
![]() Improving front-desk accuracy
Improving front-desk accuracy
During registration, the front desk must collect the right patient information, insurance details and any required documents. Accurate front-end work reduces errors that could lead to claim rejection later.
![]() Obtaining prior authorization correctly
Obtaining prior authorization correctly
Many procedures require insurance approval before the service is provided. If authorization is missing, expired or entered incorrectly, the claim may be denied.
![]() Strengthening coding quality
Strengthening coding quality
Accurate coding is essential for claim approval. Payers use diagnosis and procedure codes to process payments — wrong codes, missing modifiers or code mismatches are common denial causes.
![]() Maintaining complete documentation
Maintaining complete documentation
Clear and complete clinical documentation helps prove that the services billed were necessary and supports them. Proper documentation cuts down on denials that are caused by missing records or not enough information.
Read our blog on Denial Management Guidelines 2026 to reduce your claim rejections.
How can improved denial management maximize revenue?
![]() Get more payments back
Get more payments back
Better denial management helps providers find denied claims faster and take steps to recover money. Instead of losing revenue, more can be collected by fixing mistakes and resubmitting or appealing claims.
![]() Cut down on write-offs
Cut down on write-offs
Unmanaged denials often become write-offs — lost income. Strong denial management reduces this by improving follow-up and raising the chances of getting paid.
![]() Make reimbursement go faster
Make reimbursement go faster
A good denial management process helps teams respond to denials quickly and avoid long waits, leading to faster claim settlement and faster provider payment.
![]() Improve cash flow
Improve cash flow
When claims are settled faster and fewer bills go unpaid, the organization receives more money — keeping cash flow healthy and supporting daily financial operations.
![]() Cut down on recurring mistakes
Cut down on recurring mistakes
Denial management helps identify common errors — coding issues, missing authorization or incomplete documentation. Once found, these problems can be fixed so the same denials don't keep happening.
![]() Make operations more efficient
Make operations more efficient
A structured denial management process makes it easier to review, correct and follow up on denied claims — reducing confusion, saving staff time and making the billing process more organized.
Better denial management makes the whole revenue cycle stronger by increasing payment recovery, lowering avoidable losses and increasing revenue overall.
What does a denial management specialist do?
A denial management specialist reviews denied claims and works to recover reimbursement. Their responsibilities typically include:
 Analyzing denial reasons
Analyzing denial reasons Correcting billing errors
Correcting billing errors Preparing appeals
Preparing appeals Contacting payers for follow-up
Contacting payers for follow-up Tracking deadlines
Tracking deadlines Documenting updates
Documenting updates Reporting denial trends
Reporting denial trends Coordinating with coders, billers and providers
Coordinating with coders, billers and providers
They are essential for protecting revenue and improving claims performance.
Where can you find reliable denial management services?
When evaluating a denial management service provider, look for these core capabilities:
![]() Denial analysis and categorization
Denial analysis and categorization
A reliable provider should carefully review denied claims and sort them by reason — eligibility, coding, authorization or documentation — helping organizations identify and address the most common denial types.
![]() Claim correction and resubmission
Claim correction and resubmission
Reliable services should correct errors in denied claims and resubmit them correctly. This helps providers get paid faster and reduces the chance of another denial.
![]() Appeals management
Appeals management
Some denied claims need a formal appeal. A strong denial management team should write appeal letters, include supporting documents and submit them on time.
![]() Payer follow-up
Payer follow-up
Regular follow-up with insurance companies is critical. A good service provider should monitor every claim closely until payment is received or the issue is fully resolved.
![]() KPI tracking and reporting
KPI tracking and reporting
These factors matter because they help providers choose a denial management service that not only resolves denied claims but also improves collections, reduces revenue loss and supports long-term financial growth.
Final thoughts
Managing denials is an important part of billing and managing the revenue cycle in healthcare. It helps providers get paid for claims that haven't been paid, cut down on recurring billing mistakes and improve financial performance.
A robust denial management process extends beyond resolving rejected claims. It helps healthcare organizations set up a proactive system that stops denials, boosts reimbursement and supports long-term revenue growth.
Looking for trusted Denial Management Agents?
I've been streamlining RCM staffing since 1999.